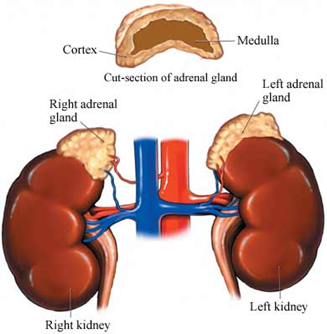
Basic Anatomy of the Adrenal Glands
The adrenal glands consists of 2 regions:
1) Adrenal Cortex
- Outer region
- Encapsulates the medullary region
- Secretes: Steroid hormones (corticosteroids, mainly C19, C21)
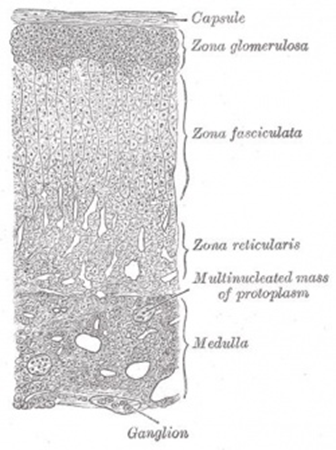
2) Adrenal Medulla
- Inner region
- Composed of: modified sympathetic ganglion cells (nervous)
- Secrets: Epinenephine & norepinephrine (catecholamines)
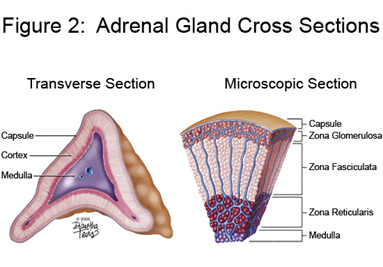
Adrenal Cortex
It contains cells with large amounts of smooth endoplasmic reticulum (SER) and abundant lipids for the biosynthesis of steroid hormones.
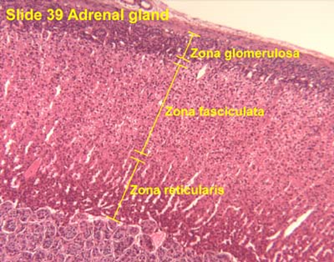
Adrenal cortex is divided into 3 zones:
1) Zona Glomerulosa
- Outermost
- Arrangement: Whorl of cells
- Steroid hormone:
-Mineralocorticoids (Aldosterone, deoxycorticosterone)
2) Zona Fasciculata
- Middle
- Arrangement: Linear Cords
- Steroid hormone:
-Glucocorticoids (Cortisol, corticosterone)
-Androgens (dehydroepiandrosterone DHEA, androstenedione)
3) Zona Reticularis
- Innermost
- Arrangement: Netlike
- Steroid hormone: Glucocorticoids & Androgens
Production of Steroid hormones
ENZYMES INVOLVED:
- hydroxylase (require O2 & NADPH)
- dehydrogenase
- isomerase
- lyase
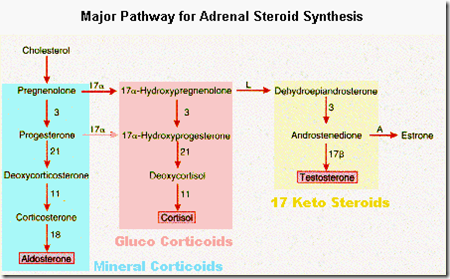
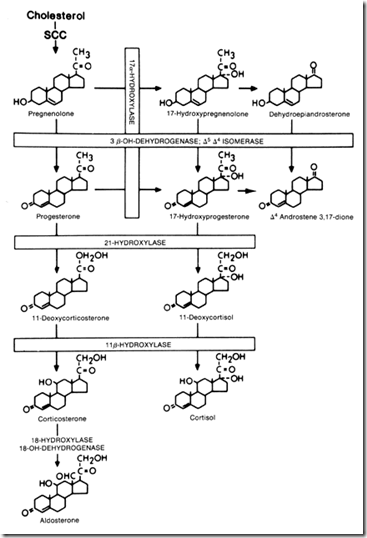
EXAMPLE: Biosynthesis of Cortisol (Chain reaction)
In Cytoplasm, Cholesterol + Acetate = Cheolesteryl esters stored in storage vacuoles.
Cholesteryl esters —b/d—> Fatty acid + Cholesterol
1st step : Cholesterol enter mitochondrion ––enzyme desmolase/ SCC—> convert to Pregnenolone (RATE LIMITING STEP)
2nd step : Pregnenolone enters cytoplasm —enzyme dehydrogenase, isomerase —> Progesterone —-> Enter Endoplasmic reticulum
3rd step : Progesterone — enzyme hydroxylase —> 17 a- hydroxyprogesterone
4th step : 17a-hydroxyprogesterone — enzyme hydroxylase —> 11-Deoxycortisol
5th step : 11-Deoxycortisol enters mitochondrion — enzyme hydroxylase —> Cortisol —-> Enter cytoplasm
RULE OF THUMB:
The production of steroid hormone depends on the enzymes available in the zone (eg mineralocorticoid produced in zona glomerulosa depends on the enzyme available to enable the chain reaction).
These hormones are released into the blood plasma when they are made (very little storage in the adrenal cell). Therefore, it can be said that the hormones are synthesized only when needed, with immediate secretion into the blood circulation.
The enzymes produced will initiate their actions by combining with specific intracellular receptors forming a complex. This complex then binds to specific regions of DNA to regulate gene expresion.
_____________________________________________________________________
Mineralocorticoids
Function:
- Regulation of the electrolyte concentrations in ECF (Na+ & K+)
Aldosterone
- Most potent mineralocorticoids (95% of mineralocorticoids produced)
- No specific plasma carrier protein, forms weak association with albumin.
- Due to lack of specific plasma carrier protein, aldosterone is rapidly cleared from plasma by liver (form tetrahydroaldosterone 3-gluocronide) which will be excreted in the urine.
When needed to retain Na+ in the body (eg. low BP), aldosterone will act on distal parts of the kidney where it will stimulate reabsorption of Na+ by increasing the no. of apical membrane Na+ channel. Therefore increase in intracellular Na+ and decreased osmolality in the kidney tubules, will cause osmosis water to be reabsorbed (osmotic pull). Corresponding to the example of decreased BP, water retention will be able to prevent further decrease of BP.
For the Na+ to be reabsorbed, Na/K pump will require ATP which will be generated by mitochondrial enzymes (mitochondrial activity increased by aldosterone), therefore Na+ will be reabsorbed, and K+ will be eliminated instead. Therefore, there will be alterations in the acid-base balance of the blood. Loss in basic content (K+) will cause blood to be more acidic.
Kidney however will compensate by secreting K+, H+ and NH+.
It does not only act on kidney tubules for Na+ reabsorption, but also on blood vessels (perspiration), tongue (saliva) and stomach (gastric juice).
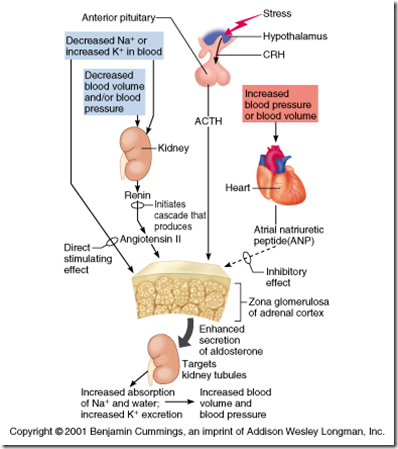
How is aldosterone release regulated?
1) Renin-Angiotensin-Aldosterone system
When the blood pressure is low, the juxtaglomerular apparatus will detect it from the amount of blood filtered into the Bowman’s Capsule, hence releasing Renin. Renin will convert Angiotensin(from liver) to Angiotensin 1. Angiotensin 1 will then be converted to Angiotensin 2 by the Angiotensin-converting-enzyme (from lungs, endothelial cells & plasma). Angiotensin 2 will act on endothelial cells (causing vasocontriction) and zona glomerulosa (secretion of aldosterone).
2) Low Na+ / High K+ via Na-K Pump
Aldosterone release to conserve Na+ and eliminate K+.
3) ACTH
Stress will cause release of corticotropin releasing hormone (CRH) from hypothalamus —-> Adrenocorticotropin (ACTH) from anterior pituitary —-> act on adrenal gland —-> produce aldosterone.
Aldosterone release will cause increase in blood volume & BP, ensuring adequate delivery of O2/CO2 and nutrients during stressful period.
4) Atrial Natriuretic Factor (ANF) – INHIBITORY
When blood pressure rises in the atrium of the heart, ANF will be produced and block the renin and aldosterone secretion. Therefore, Na+ will not be reabsorbed, hence causing more water loss. Therefore, the b
lood pressure can be decreased from decreased blood volume.
Summary:
Aldosterone hypersecretion:
Aldosteronism (Retention of Na+)
- Hypertension
- Hypernatremia & Hypokalemia
- Alkalosis
Aldosterone hyposecretion:
Addison’s disease (discussed in another post)
_____________________________________________________________________
Glucocorticoids
Circulates in plasma (protein-bound/free form)
- Plasma binding protein : α-globulin/ transcortin/corticosteroid-binding globulin (CBG) produced in the liver (increased synthesis by estrogens)
- Only small amounts bound to albumin (weak association)
- Unbound: 8% of total cortisol (biologically active)
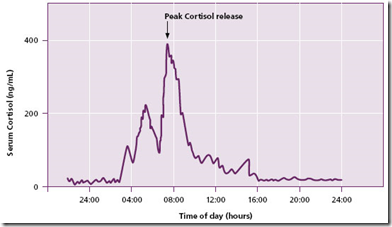
Secretion dependent on CRH —> ACTH (stress hormone) —-> Cortisol which occurs periodically regulated by the diurnal rhythm (certain timing) of ACTH release.
Peak plasma cortisol & ACTH (same pattern) level will be around 7am, just before waking up. Cortisol level will gradually decrease and will be at it’s lowest during sleep. Then it will start increasing again before waking up.
Effects of Cortisol
It will increase basal metabolism.
- Increase glucose production by liver (by increasing delivery of amino acids from peripheral tissues, increase gluconeogenesis by increasing amount of enzymes, and permitting other key metabolic reactions to operate at maximal rate)
- Inhibit glucose uptake (except brain & heart)
- Increase hepatic glycogen deposition
- Promote lipolysis in extremities & lipogenesis in other sites (face & trunk) – clinical feature of Cushing’s
- Promote protein & RNA metabolism (anabolic, subsequently catabolic b/d protein)
Weaken host defense mechanism
- Suppress the immune response
- Lysis of lymphocytes
- Decrease no. of circulating leukocytes, migration of tissue leukocytes
- Inhibit fibroblast proliferation
- Induce lipocortins –> inhibit phospholipase A –> inhibit production of inflammatory molecules (prostaglandin, leukotrienes)
Increase blood pressure (during stressful periods)
- Cause release of aldosterone –> Na+ retention –> water retention
- **However also necessary for maintenance of normal BP & CO. Inhibition of ADH release will cause increased urination to balance aldosterone release.
Mimic aldosterone action
- Binds to aldosterone receptors —> aldosterone action
Inhibit ADH release
- Binds to cortisol receptors —> inhibit ADH release —> increase in free water loss —> polyuria.
Cortisol hypersecretion:
Cushing’s Syndrome
- persistent hyperglycemia (high glucose)
- loss in muscle & bone protein
- water & salt retention (hypertension, oedema) – aldosterone action
- swollen ‘moon’ face
- buffalo hump
- tendency to bruising
- poor wound gealing
- enhanced anti-inflammatory effects (lack of inflammatory cells)
- polyuria, polydipsia – Low ADH
- striae
- pendulous abdomen
Cortisol hyposecretion
Addison’s disease (same as mineralocorticoid hyposecretion)
- deficiency in both glucocorticoids (cortisol) & mineralocorticoids (aldosterone)
- weight loss
- plasma glucose & natrium level decrease
- severe dehydration (thru loss of Na)
- hypotension
_____________________________________________________________________
Gonadocorticoids (Sex Hormones)
- Precursors: Androsterotenedione, DHEA, DHEA-sulphate
- Conversion to active androgens: testosterone & dihydrotestosterone (DHT)
- Androgens important precursors of oestrogens for post-menopausal women (ovaries regressed)
- Release stimulated by : ACTH (but no –ve feedback on ACTH release)
Gonadocorticoids hypersecretion:
Masculinisation/Virilisation
Prepubertal males:
- rapid maturation of reproductive organs & appearance of 2ndary sex characteristics
- high sex drive
Females: Androgenital syndrome
- Develop beard
- Masculine pattern of body hair distribution
- Clitoris grows to resemble small penis
- Also linked to Polycystic Ovarian Syndrome (another post)

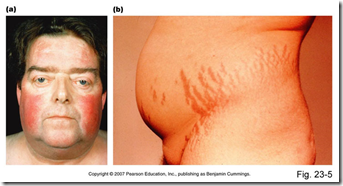
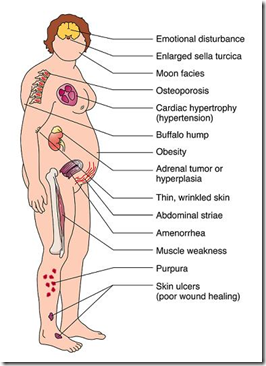

The pictures for Addison’s I believe are actually for Cushing’s, but the description is correct. To verify: http://www.as.miami.edu/chemistry/2086/Chap18/Adrenal%20glands%20-%20end.html uses one of your pictures.
Thank you for the great post, by the way!
Awesome!!!!!
Thanks for sharing about harmones Hormones Medicine Exporter Supplier India